

In the UK, the Caldicott Principles set the gold standard for safeguarding patient data. These eight principles ensure that confidential information is handled securely, shared appropriately, and used only when absolutely necessary in health and social care settings.
If you want to explore the concept further, read on to the end to deepen your knowledge!
This guide covers the following aspects:
- What the 8 Caldicott Principles are
- How they align with UK laws like GDPR
- The role of Caldicott Guardians in upholding these standards
- How to apply these principles in practice
What Are the Caldicott Principles?
The Caldicott Principles are guidelines for protecting patient information in health and social care settings. They ensure that confidential patient data is:
- Used only when necessary
- Kept to the minimum needed
- Accessed only by those who need it
- Shared properly when required for care
Background
Established in 1997 by Dame Fiona Caldicott, the Caldicott Principles were created to protect patient information within the healthcare system. Originally comprising six key guidelines, the framework evolved. Two additional principles were introduced in 2013 and 2020 to strengthen data protection measures.
By 2021, the UK’s National Data Guardian formally mandated these principles, ensuring implementation across NHS organisations, hospitals, clinics, social care services, and any third parties involved in managing confidential patient data. This reinforced their role in maintaining patient trust and upholding privacy standards in healthcare.
What Is Patient-Identifiable Information?
What Is Patient-Identifiable Information?
The Caldicott Principles protect any data that can identify a patient, including:
- Name, address, date of birth, NHS number
- Medical history, test results, diagnoses
- Photos, recordings, or unique conditions
- Any details that could indirectly reveal identity
This includes deceased patients’ records, as confidentiality duties continue after death.
Why Are These Principles Important?
Proper handling of patient information is crucial to avoid data misuse, identity theft, and breaches of patient trust.
Builds Patient Trust – Ensures patient confidence that their data won’t be misused.
Balances Privacy & Care – Helps staff share information when needed without violating privacy laws.
Ensures Legal Compliance – Helps meet UK GDPR and Data Protection Act 2018 requirements.
Prevents Data Breaches – Protects organisations from reputational damage and legal penalties.
The 8 Caldicott Principles
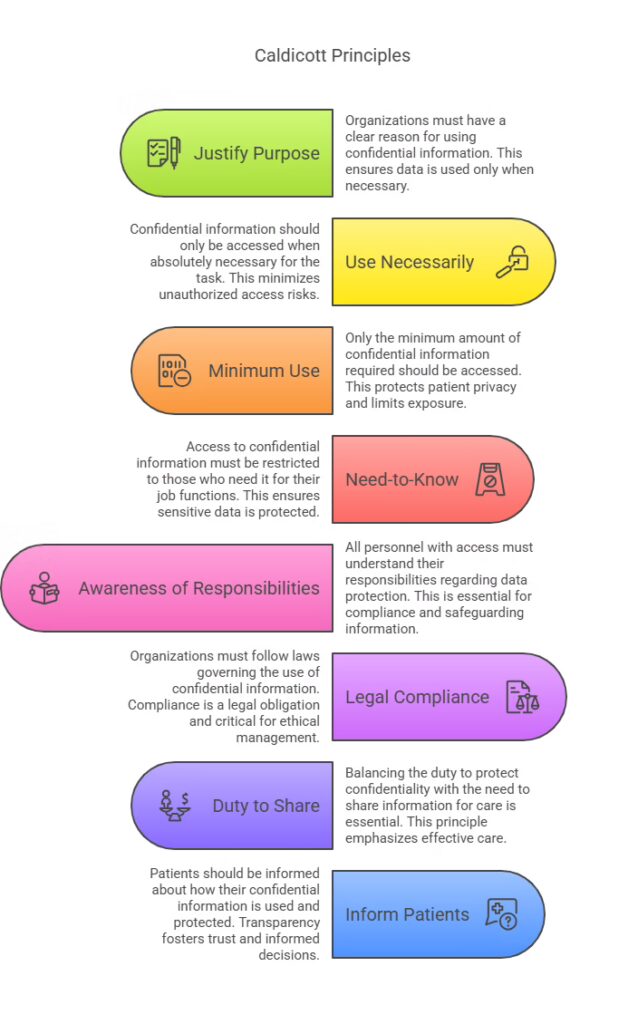
Each principle guides healthcare professionals in handling patient data responsibly. Before exploring the details, here is an overview of all eight Caldicott Principles as of 2024 :
Principle 1: Justify the Purpose for Using Confidential Information
Before accessing or sharing a patient’s confidential data, there must be a clear and valid reason. Every use of confidential information should be evaluated, documented, and justified.
Healthcare professionals cannot access records simply out of curiosity. The purpose must be specific and approved by relevant authorities, such as a Caldicott Guardian or ethics committee. Regular reviews should also be conducted to ensure the continued necessity of the data use. If it is no longer required, access should stop immediately.
This principle helps prevent unauthorised access and creates an audit trail to track who accessed the data and why. It was introduced to address concerns that patient records were sometimes accessed without proper justification. Enforcing this rule reduces snooping and misuse, making it a critical safeguard for privacy.
Before handling patient information, always ask: “Do I have a valid reason?” If the answer is unclear, you should not proceed. Confidential data should only be used for patient care, safety, or another ethical, approved purpose, never for personal curiosity.
The NHS systems require staff to select and log a reason for accessing a record (e.g., “direct care of the patient”). This accountability measure reflects Principle 1 in action.
Principle 2: Use Confidential Information Only When Necessary
Even when there is a justified reason to access patient data, it should only be used if necessary. If a task can be completed without using identifiable information, that alternative should always be chosen.
Before accessing confidential information, consider the following:
Can I achieve my goal without patient-identifiable data?
Would anonymised or coded data be enough?
If the answer is yes, then personal details should not be used.
A hospital analysing treatment success rates does not need patient names or NHS numbers. Instead, they can use anonymous statistics (e.g., “85% of patients recovered in two weeks”).
In short, this principle promotes data minimisation and the use of de-identified data for research, audits, and training. If personal details are unnecessary, using them increases risk with no added benefit.
Principle 3: Use the Minimum Necessary Personal Information
When handling patient data, only the essential details should be accessed or shared. More information does not mean better care; it just increases risk.
For instance, a community nurse referring a patient to a social worker should only share relevant details about the patient’s health and needs. The entire medical history is not necessary.
A clinic referring a patient to a specialist should include:
✔ The current condition being treated.
✔ Relevant medical history (only related to the issue).
✔ Current medications and allergies.
❌ Unrelated past medical history (e.g., an old knee surgery for a heart specialist).
Sharing more data than required increases the chance of breaches. Using role-based access in healthcare IT systems ensures that only necessary information is available to each professional.
Principle 4: Access Should Be on a Strict Need-to-Know Basis
Not everyone working in healthcare needs access to all patient records. Access should be strictly limited based on job roles and necessity.
Here are some of the examples for better understanding:
A receptionist needs to see appointment details but should not access medical histories.
A lab technician should only see test results, not full patient files.
A doctor treating the patient needs to review the entire medical history but does not need billing details.
Modern electronic health record (EHR) systems use role-based access controls to enforce these restrictions. Unauthorised access is flagged, and any suspicious activity is tracked.
In some cases, employees have been fined or dismissed for accessing celebrity or family members’ medical records without authorisation.
Principle 5: Everyone With Access Must Be Aware of Their Responsibilities
Confidentiality policies and security controls only work if staff follow them. Anyone with access to patient data must understand their responsibilities.
For example, a nurse discussing a patient’s case should ensure they are not overheard in public areas. Similarly, a ward clerk printing discharge papers must hand them to the correct patient.
Key responsibilities are:
✔ Completing data protection training regularly.
✔ Understanding NHS confidentiality policies and UK privacy laws.
✔ Reporting breaches or suspicious activity immediately.
Many data breaches occur due to human error, such as sending information to the wrong person or leaving records unsecured. Organisations must practise a culture of confidentiality through training, clear policies, and accountability measures.
Principle 6: Comply with the Law
Handling patient data is a legal requirement. Several UK laws regulate data protection, including:
- UK GDPR (General Data Protection Regulation)
- Data Protection Act 2018
- Common Law Duty of Confidentiality
- Freedom of Information Act 2000 (with personal data exemptions)
A hospital must obtain patient consent before sharing records outside the care team. If data is shared without consent, it must be under a legal exemption, such as a court order or statutory reporting requirement.
Failure to comply with these laws can result in legal action, fines, and reputational damage. Healthcare organisations must have policies and security measures in place to meet legal obligations.
Principle 7: The Duty to Share Information is As Important As the Duty to Protect It
While confidentiality is crucial, withholding necessary information can be harmful. In some cases, sharing patient information is essential for their safety and care.
One such scenario can be when a patient in a mental health crisis is at risk of self-harm, their GP, psychiatrist, and emergency services must share relevant details to ensure urgent support.
Sharing information is especially important when multiple professionals are involved in a patient’s care. This principle ensures that the fear of breaching confidentiality does not lead to care delays.
However, information should still be shared appropriately, only with those who need to know and within legal and ethical guidelines.
Principle 8: Inform Patients About How Their Information Is Used
Patients have the right to know how their data is collected, stored, and shared. Transparency builds trust and ensures individuals feel in control of their information.
How to inform patients:
Provide privacy notices in GP surgeries and hospitals.
Explain when and why data is shared (e.g., for research, treatment, or audits).
Offer opt-out options where possible.
Some healthcare organisations also offer patient portals where individuals can see who has accessed their records and why. NHS Digital provides a data opt-out system, allowing patients to choose whether their records can be used for research purposes.
Applying the Caldicott Principles in Practice
How do you ensure compliance with these principles in daily healthcare work?
1. Use Checklists & Mnemonics
FIONA C + Share & Inform
F – Formal justification for using patient data
I – Information only when necessary
O – Only use the minimum required
N – Need-to-know basis for access
A – All staff must be trained
C – Comply with the law
2. Implement Role-Based Access Controls
- Restrict system access so that staff only see relevant data.
- Use login credentials to track who accesses records.
- Prevent unauthorised staff from accessing private details.
3. Provide Regular Confidentiality Training
- Annual training sessions on data protection.
- Simulated scenarios to test staff knowledge.
- Posters and reminders about confidentiality rules.
4. Use Data Minimisation & Anonymisation Techniques
- Anonymise data for non-care purposes (e.g., research).
- Use pseudonyms or coded identifiers instead of patient names.
- Limit access to non-essential details.
5. Involve the Caldicott Guardian
- Seek advice when unsure whether to share or withhold patient data.
- Consult the Guardian for difficult confidentiality decisions.
- Ensure all staff know who the Caldicott Guardian is in their organisation.
The Role of the Caldicott Guardian
A Caldicott Guardian is a senior professional in a healthcare or social care organisation responsible for protecting patient confidentiality and ensuring personal data is handled correctly. Their role is to balance privacy with the need to share information safely when necessary for patient care.
What Does a Caldicott Guardian Do?
- Advice on Sharing Patient Information – They help staff decide when and how to share patient data while following privacy laws and ethical guidelines.
- Ensures Compliance – They make sure the organisation follows NHS rules, GDPR, and the Data Protection Act 2018, ensuring all data is handled legally and securely.
- Investigates Data Breaches – If patient data is misused or leaked, they step in to assess the situation and recommend steps to prevent it from happening again.
- Improves Policies – They help create and update rules on how patient information is stored, used, and shared to keep it secure and protect privacy.
Further Learning: Recommended Courses
If you work in health or social care, consider professional training in courses like the Level 3 Diploma in Health and Social Care, Level 3 Diploma in Nursing Assistant Complete Training, Care Certificate (Standards 1–15) Bundle or Adult Safeguarding Level 3 Online Course.
FAQ
What is the Caldicott Principle 8?
Caldicott Principle 8 states that patients must be informed about how their confidential data is used, ensuring transparency and trust.
What are the 8 Principles of Information Governance?
The eight Caldicott Principles ensure the responsible handling of confidential patient data, focusing on justification, necessity, minimisation, restricted access, accountability, legal compliance, appropriate sharing, and transparency.
What are the Caldicott Principles?
The Caldicott Principles are guidelines for handling patient information responsibly, ensuring confidentiality, security, and lawful data use in healthcare.
What is Caldicott Principle 7?
Caldicott Principle 7 states that the duty to share information is as important as the duty to protect it, ensuring patient safety is not compromised by excessive data restrictions.
Conclusion
In the modern world, trust is also a key component of patient information protection. When you see a doctor, you anticipate that your personal information will be kept private and used exclusively to provide care. That is made possible by the Caldicott Principles, which instruct medical personnel on how to appropriately manage sensitive data.
Organisations may prevent data breaches, preserve patient privacy, and strike the ideal balance between acceptable information sharing and confidentiality by adhering to these guidelines. Because there is a person behind every record who deserves to feel safe and secure, protecting patient data is ultimately about respect.




 " alt="The 6 Principles of Safeguarding: Protect Before Harm Happens" />
" alt="The 6 Principles of Safeguarding: Protect Before Harm Happens" />
 " alt="Personal Development Goals: 5 Meaningful Examples That Work" />
" alt="Personal Development Goals: 5 Meaningful Examples That Work" />
 " alt="TILE in Manual Handling: Meaning, Checklist & Safer Lifting Guide" />
" alt="TILE in Manual Handling: Meaning, Checklist & Safer Lifting Guide" />